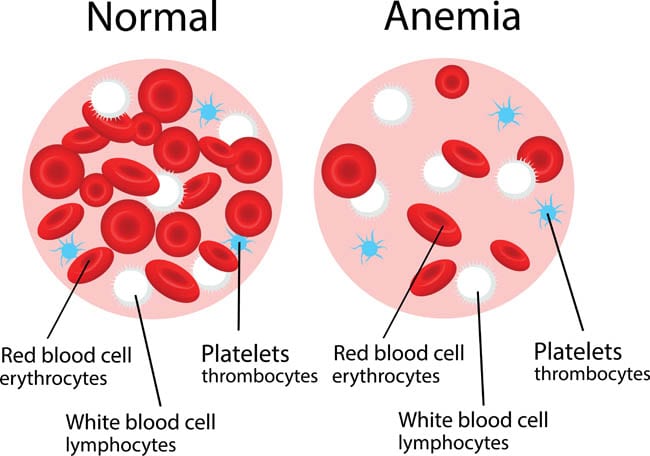
Blood consists of red blood cells, white blood cells and plasma. The red cells carry oxygen and their well-being is essential for life. Red blood cells, like most other components of the body, are made of protein, and proteins can be recognized and destroyed by the body’s immune system.
Blood Types
An A-B system is used in cats. The cat has essentially two blood groups: A and B (although there is a third, very rare, group, AB, which is a combination of the two). The red blood cell proteins are:
Type A antigen = N-glycolyl-neuraminic acid
Type B antigen = N-acetyl-neuraminic acid
Type AB antigen = an equal amount of both proteins
A-B blood groups are inherited in a simple dominant form. Group A is dominant over B (in most cases), hence Type A cats may be homozygous AA or heterozygous AB. Type B cats must be homozygous BB. The exception to the rule is the AB blood group which is very rare, but in which A and B appear to express co-dominance.
The frequency of feline blood groups is subject to geographic variation as the ratio of all feline blood types varies from country to country. In the United States, approximately 99% of domestic cats are Type A. In the United Kingdom it is 87% and in Australia it is about 73%.1
Type B blood is usually seen in purebred cats. The following list shows the breeds and their frequency.1
- Siamese and related breeds, Burmese, Tonkinese, Russian blues show no incidence of Type B blood.
- Maine Coon, Norwegian Forest, Domestic Shorthair (DSH), Domestic Longhair (DLH) show 1-10% incidence.
- Abyssinian, Birman, Himalayan, Persian, Japanese Bobtail, Somali, Sphinx, Scottish Fold show 11-20% incidence.
- Exotic and British shorthairs, Cornish and Devon Rex show 20-45% incidence.
- There are a handful of purebred cats for whom blood type B frequency has not been determined.
Type AB blood occurs in the United States and Australia at about 1%, and in the United Kingdom at 5%. Breeds that have exhibited this blood type are DSHs, Scottish Folds, Birmans, British Shorthairs, Somalis, Bengals, and Abyssinians.1
Transfusions
A transfusion is a transference of whole blood or a blood component of one animal into the vascular system of another. The main aim of blood transfusions is to increase the PCV of a severely anemic (deficiency of red blood cells) cat while erythropoiesis (development of mature red blood cells – erythrocytes) hopefully proceeds to restore red cell numbers and resolve the anemia. They are also utilized when extreme blood loss has occurred either externally or internally.
Approximately 4-5% of a cat’s body weight or about an ounce per pound is composed of blood. An average 10 pound cat has about 8-9 ounces in his body. If a cat reaches a loss of about 25% of his normal blood volume, he will go into a state of shock (bodily collapse or near collapse caused by inadequate oxygen delivery to the cells). A transfusion of whole blood gives the recipient a new supply of red blood cells increasing the oxygen-carrying capacity in the cat’s blood stream. Other blood components provide fluid replacement, helpful in the prevention or treatment of shock, although this can also be accomplished without a transfusion.
In the cat world there is no such thing as a “universal donor”. Typing is required when transfusing cats even though the majority possess Type A blood. Blood group B cats lack a hydroxylase enzyme that converts the N-acetyl-neuraminic acid to N-glycolyl-neuraminic acid. Because of this, even a small amount of the wrong blood type may kill a cat. Type AB cats lack naturally occurring antibodies and therefore can safely receive blood from either Type A or B cats and are considered “universal recipients”.
- Transfusing Type A blood to a Type A cat – transfused blood lasts between 29-39 days
- Transfusing Type A blood to a Type B cat – transfused blood lasts about 1.3 hours. There is rapid destruction of the donated Type A blood with severe clinical signs: hypotension (low blood pressure), defecation, vomiting, hemoglobinemia (a medical condition in which free hemoglobin proteins are present in blood plasma, this occurs when red blood cells within which hemoglobin is normally found have been injured while in the blood vessels), neurologic depression and even death.
- Transfusing Type B blood to a Type A cat – transfused blood lasts 2.1 days. Mild clinical signs.
Any cat requiring further transfusions would need to be cross-matched with any subsequent donor, even one of the same blood type, as the first transfusion may result in antibody production against erythrocyte antigens other than those of the A-B system. The donor blood is also tested to be free of any retroviruses and FIA (Feline Infectious Anemia is a blood disease caused by the rickettsial parasite, Hemobartonella felis).
Oxyglobin
Oxyglobin® is the first and only oxygen therapeutic to receive marketing clearance from the U.S. FDA and the European Commission for veterinary use. It is produced by Biopure Corporation. The product is indicated for the treatment of canine anemia regardless of the cause. However, many veterinarians have used it successfully to treat cats since 1998. Anemia is a potentially life-threatening condition that affects millions of pets each year. Oxyglobin is a sterile, intravenously administered solution consisting of chemically stabilized hemoglobin (the protein that carries oxygen) in a balanced salt solution. Unlike blood, it does not contain red blood cells. Instead, it contains cross-linked hemoglobin molecules that circulate in plasma and immediately transport oxygen to tissues upon infusion. Since it does not contain red blood cells, cross-matching feline blood types in an emergency situation is not necessary. It is especially helpful in cats that are Type B or AB when there is no donor blood available. However, once transfused, it is only effective for one or two days. It is used strictly to stabilize the patient while the cause and treatment can be determined. Additionally, it is not useful in cases of chronic (long-term or recurring) anemia. In these cases red blood cells are needed.
Neonatal Isoerythrolysis
Type A blood is dominant over Type B blood. When a Type A tom cat mates with a Type B queen, the kittens will all be Type A blood or rarely Type AB. However, the Type B antibodies to Type A blood in the mother cat are passed in the colostrum (milky fluid produced for 1-2 days after birth) and milk to the Type A kittens. Neonatal isoerythrolysis results as the kittens’ red blood cells are destroyed by the Type B alloantibodies (naturally occurring antibodies directed against foreign feline blood group antigens). Clinical signs include jaundice (yellowing of the skin and the whites of the eyes caused by an accumulation of bile pigment (bilirubin) in the blood), red-brown urine, and rapid death. This form of hemolytic anemia may be reversed. Neonatal isoerythrolysis is a factor of Fading Kitten Syndrome in purebred cats.
Fading Kitten Syndrome
With Fading Kitten Syndrome the kittens appear healthy and vigorous at birth, but some kittens suddenly die after nursing while others “fade” and die 3-7 days later. The fading kittens stop nursing, become pale or jaundiced due to red blood cell destruction, and have red-brown urine. The red-brown urine distinguishes Neonatal isoerythrolysis from all other causes of the Fading Kitten Syndrome. Breeders should check all kittens for red-brown urine during the first 2 days of life. The diagnosis of Neonatal Isoerythrolysis (NI) is confirmed by blood typing the tom and queen, or the queen and kittens. Once the symptoms of NI are noticed, some kittens may be saved by a transfusion of red blood cells (RBCs) from the queen. Since the queen’s blood contains anti-A alloantibodies, the RBCs must be thoroughly washed with saline to remove these antibodies. The washed RBCs are given intraperitoneally (within the abdominal membrane) 5 ml per kitten. Surviving kittens usually recover to full health but may develop necrosis (localized death) of the tail tip at 2 weeks of age.
Blood Typing Your Cat
A rapid card agglutination test allows a quick and easy in-house blood typing for cats at your veterinarian’s office. Anyone considering breeding pedigree cats that fall into the Type B category should first have their veterinarian perform a blood typing test.
Blood Banks and Donor Cats
Many veterinary clinics house donor cats that belong to the hospital and are considered resident donors. They are the pets of the clinic and are treated very well. Such donors are there to provide a quick supply of whole blood when needed. However, in-hospital supplies may be low or specialized blood products may be required. Blood banks and their distribution centers handle this need.
Currently, there are four animal blood banks in the United States. They periodically conduct blood drives to replenish their inventory of blood and blood products. However, because of the prevalence of infectious diseases in cats, such as Feline Leukemia (FeLV), the feline immunodeficiency virus (FIV) and the feline infectious peritonitis virus (FIP) blood banks must be very selective in choosing donors.
The blood bank does not have absolute knowledge of a feline donor’s previous exposure to disease, and testing does not always rule out the possibility of infectious diseases. Animal Blood Resources International is headquartered in Dixon, Calif., and also operates out of a Stockbridge, Michigan, facility. They service over 65% of all veterinary transfusion needs in the United States. Instead of conducting blood drives it obtains its inventory from about 25 cats kept in a well cared for isolated colony at the blood bank. After the cats have completed one year of donor service they are adopted out. All of their cats come from the local shelters and humane societies.
1 – Cynda Crawford, DVM, University of Florida, College of Veterinary Medicine.
Information on this site is for general information purposes only and is provided without warranty or guarantee of any kind. This site is not intended to replace professional advice from your own veterinarian and nothing on this site is intended as a medical diagnosis or treatment. Any questions about your animal’s health or diet should be directed to your veterinarian.
© 2022 Feline Nutrition Center. All Rights Reserved.
Privacy | Terms