Vaccines are given to prevent specific viral infections. They cause the immune system to produce antibodies that combat viruses. If the cat comes into contact with the virus at a later time its body can now fight it off.
Your cat should be vaccinated against disease whether it is an indoor or outdoor cat. Some vaccines may not be required if the cat is strictly indoors all of the time. Diseases can be airborne and ingested through respiration or transmitted through direct or indirect contact such as biting, sexual contact, or contaminated materials.
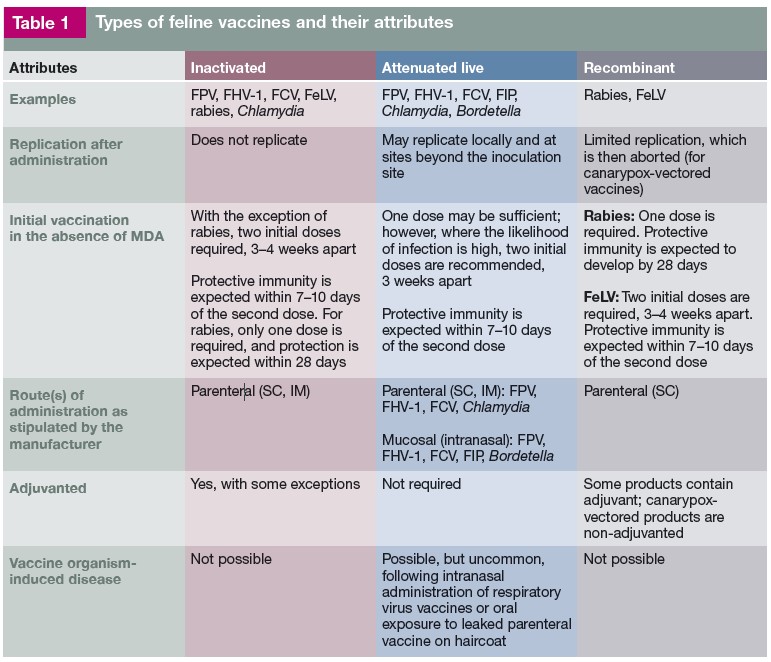
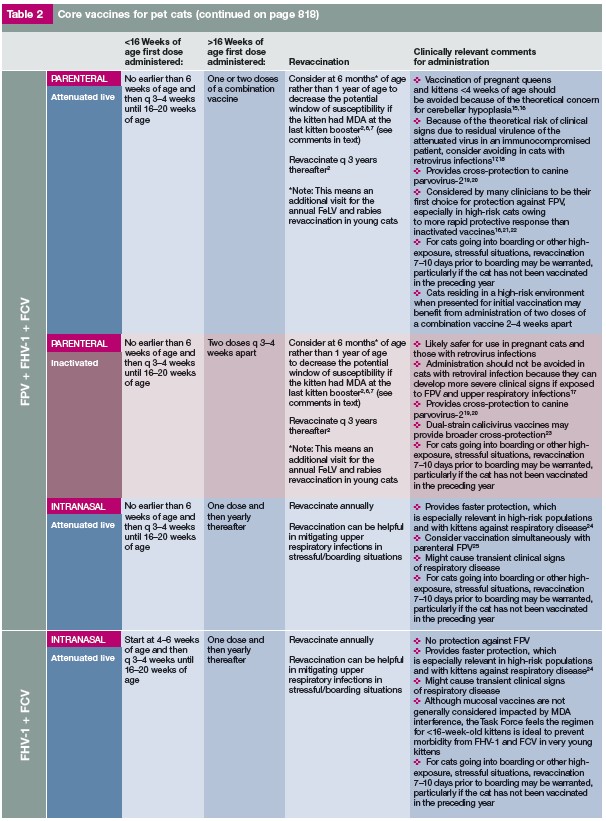
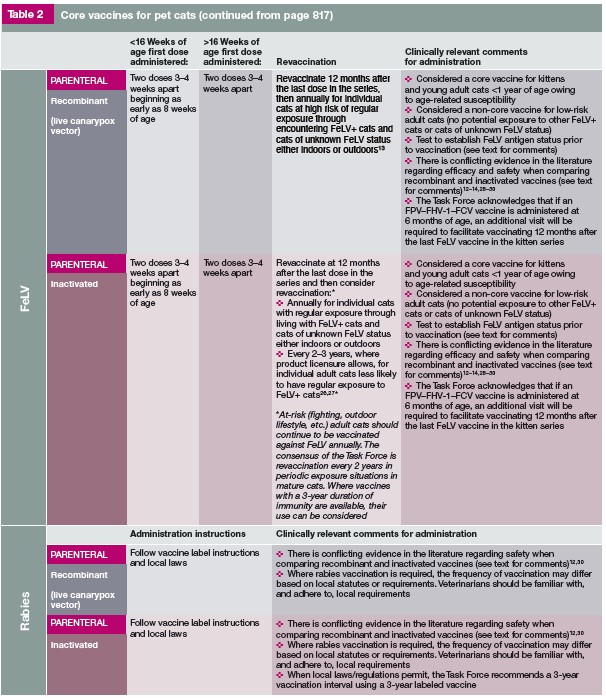
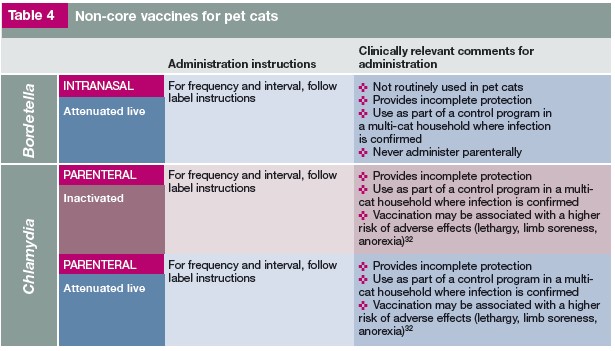
Below are tables from the 2020 guidelines that were prepared by a Task Force of experts convened by the American Animal Hospital Association (AAHA) and the American Association of Feline Practitioners (AAFP) and were subjected to a formal peer-review process. This is intended as a guideline only, not an AAHA or AAFP standard of care. For more information see the AAHA/AAFP article from the Journal of Feline Medicine and Surgery (2020) 22, 813-8301. It had been years since feline vaccines have been evaluated for usage and time intervals for boosters. For more information on vaccine guidelines for vaccines given to breeding cats, kittens, and cattery animals please see the full Report1. Following the vaccine table is a section on the diseases that the vaccines are preventing or alleviating.
If your cat has no vaccine history, all of the vaccines should be given to your cat: FHV-1, FCV, FPV (herpesvirus, calicivirus, parvovirus respectively) often combined into one injection (FVRCP-Feline Viral Rhinotracheitis, Calicivirus, Panleukopenia) and rabies. The feline leukemia vaccine should only be given after a leukemia test has been performed. If the cat tests positive for feleuk then there is no benefit to giving the vaccine to the cat. It is typically only given to cats that reside outdoors or have contact with outdoor cats. Vaccinating for FCV and FHV-1 does not prevent contraction of the disease but it does show more than a 50% reduction in the severity of the symptoms1. FPV vaccines generally provide complete protection from the infection as a result of antibodies induced by vaccination. If a cat does contract FPV and survives, it will now be immune to re-infection1.
Every cat’s vaccination schedule should be discussed with your veterinarian. As your cat ages, its health changes, or its exposure or lack of exposure to other cats alters during the course of its life, its vaccination schedule should be altered to keep pace.
Illness can decrease the immune response and cause additional physiologic stress to your cat so cats should never be vaccinated unless they are healthy.
Allergic reactions to vaccines are rare but do occur. Lethargy, collapse, diarrhea, vomiting, swelling, or itching of the face within the first 24 hours after vaccination should be reported to your veterinarian immediately. If left untreated, an extreme allergic reaction to the vaccine(s) could cause death.
Although you may only need to take your cat to the veterinarian once every three years for booster vaccines, it is still wise to bring your cat to the vet once a year for a thorough exam. The yearly exam may discover any problems you may not have noticed that will be highly treatable with early detection. It’s well worth the money you spend on yearly office visits if you detect a disease early or prevent a debilitating disease.
Vaccine Guidelines 2020
These guidelines were prepared by a Task Force of experts convened by the American Animal Hospital Association (AAHA) and the American Association of Feline Practitioners (AAFP) and were subjected to a formal peer-review process. This is intended as a guideline only, not an AAHA or AAFP standard of care. For more information see the AAHA/AAFP article from the Journal of Feline Medicine and Surgery (2020) 22, 813-830
Abbreviations: DNA (deoxyribonucleic acid); FCV (feline calicivirus); FeLV (feline leukemia virus); FHV-1 (feline herpesvirus type 1); FIP (feline infectious peritonitis); FISS (feline injection-site sarcoma); FPV (feline panleukopenia virus); Ig (immunoglobulin); IM (intramuscular); MDA (maternally derived antibodies); SC (subcutaneous); WSAVA (World Small Animal Veterinary Association)
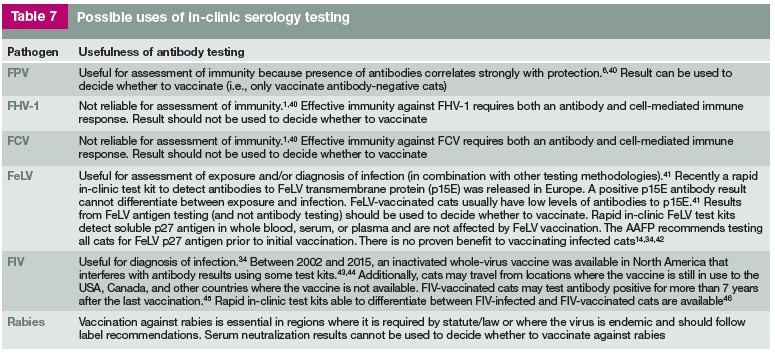

Injection Sites for Vaccine Antigens
The recommended injection sites were developed by the American Association of Feline Practitioners and the Academy of Feline Medicine1 and adopted by the Vaccine-Associated Feline Sarcoma Task Force:
FPV, FHV-1, FCV antigens: should be administered on the limbs or tail, as distally as possible
Rabies Virus antigens: should be administered on the right rear limb, as distally as possible
Feline Leukemia Virus antigens: should be administered on the left rear limb, as distally as possible
The reason for the injection sites on the limbs or tail as distally as possible is if a sarcoma forms and removal of the whole sarcoma is not possible the limb or tail may be removed to prevent metastasis to others parts of the body.
For additional Vaccine Guidelines visit Dr. Lisa Pierson’s vaccine page which discusses the common practice of overvaccination.
Feline Parvovirus
Synonyms: infectious enteritis, distemper, agranulocytosis, ataxia, panleukopenia
A highly contagious disease of cats. Symptoms include fever, anorexia (loss of appetite), depression, dehydration, reduced leukocytes (white blood cells).
All secretions and excretions of affected animals contain the virus and the infection spreads through direct contact or by material contaminated with the virus.
Cats will usually get a fever, stop eating, vomit and become depressed and weak. Diarrhea may occur. Although the cat may drink quite a lot, it will be dehydrated. The course of the disease is approximately 5 – 7 days.
Mortality (death rate) is high, especially in young cats, and losses from 60 – 90 % are reported.
Treatment entails combating dehydration, providing nutrients and electrolytes, and preventing secondary infection. Blood transfusions are useful. If the cat recovers, it will then be immune to the disease.2
Feline Herpesvirus-1 and Feline Calicivirus (FHV-1, FCV)
Synonyms: rhinotracheitis
About 40-45% of feline upper respiratory infections are a result of a herpesvirus infection. Feline calicivirus accounts for another 40-45%.
Transmission occurs by aerosol droplets and from a person contaminated with the virus from an infected cat. It may persist in an infected cat for up to 11 months where the now symptomless cat continuously sheds the caliciviruses and herpesvirus. Stress may cause a secondary attack.
Fever, frequent sneezing, conjunctivitis, rhinitis, and salivation may occur. Excitement or movement may induce sneezing. Nasal and ocular discharge increases and becomes mucous and pus like. Depression and anorexia are evident.
Signs may be exhibited from 5-10 days in mild cases and 3-6 weeks in severe cases. Mortality is low and prognosis is good except in kittens and older cats.
Use of antibiotics are helpful for secondary infections. Keep the nose and eyes clear of discharge. Nose drops may be useful but must be compounded for cats.2
Rabies
Synonyms: encephalomyelitis, hydrophobia
It is transmitted from animal to animal by means of a bite containing virus-infected saliva.
The first stage is a change in behavior. Animals stop eating and drinking. Salivation may be apparent. Animals tend to seek solitude, they may become overly friendly or affectionate or vicious.
The next stage is characterized by paralysis of the throat, salivation, and inability to swallow. The animal may once again be vicious or friendly. When vicious, cats may attack suddenly, biting and scratching viciously. Muscular incoordination, convulsive seizures, coma, and death follow. There is no cure for rabies, the animal is usually dead within 10 days.
Unvaccinated cats bitten by a known rabid animal should be euthanized immediately or put in strict isolation for no less than 4 months. If the cat has been vaccinated with a one-year vaccine, it must have been vaccinated within the previous year to be safely considered for a booster vaccine given after the bite.2
Leukemia
Associated diseases: visceral lymphoma, lymphosarcoma
Transmission occurs by cat-to-cat contact with infected saliva. Infected cats are predisposed to neoplasia or one of the nonmalignant diseases which is associated with feline leukemia virus infection.
The cat exhibits anemia, lethargy, anorexia, and wasting. There may be respiratory problems, digestive problems, and coughing.
Chemotherapy may control the lymphosarcoma and sometimes long-term remission is possible. Survival of 3-6 months is more common although some cats live longer.2
Defraying Vaccination Costs
If you can’t afford vaccinations for your pet, check into your local shelter, Humane Society, or Animal Care and Regulation Division for information on reduced cost or free vaccinations available in your area. You may also want to contact your local pet store for reduced cost vaccinations and dewormings, many have programs set up with local veterinarians.
Vaccine-Associated Feline Sarcoma
There has been a recent phenomena regarding malignant sarcomas (cancerous tumors) associated with vaccine injection sites. It was first noticed by veterinarians in 1991. The Vaccine-Associated Feline Sarcoma Task Force was formed in 1996 to research the problems associated with vaccine injection sites and in doing so institute prevention and treatment guidelines. Most veterinarians agree that the risk of your cat developing malignant sarcomas at vaccine injection sites is minimal compared to the risk of contraction of any of these diseases that may be prevented through vaccination.
Cats presenting with the sarcomas also had something else in common, they lived along the North Atlantic Coast. It was also noted that there had been an outbreak of rabies in raccoons in that region increasing the need for vaccination in cats against the disease. The feline leukemia vaccine was also becoming widely used in cats at that time and although they still don’t know why the rabies and feline leukemia vaccines cause this they believe they are responsible nonetheless.
According to Dr. James Richards, DVM and chairman of the American Veterinary Medical Association Vaccine-Associated Feline Sarcoma Task Force, the adjuvants (chemicals added to a vaccine to increase its effectiveness) may contribute to the likelihood of feline sarcomas developing. The adjuvants may contain aluminum or plant-derived materials which have been seen microscopically within tumors. These adjuvants are added to both the rabies and feline leukemia vaccine antigens.
One in approximately every 10,000 cats develops a sarcoma (fibrous tumor of connective tissue) within a few months after vaccination.1 These fibrosarcomas spread slowly and can be excised but they usually reoccur. In about 25-30% of the cases, the tumor eventually metastasizes (spreads) to other sites of the body, such as the lungs.1 The long term prognosis is not good.
The best way to reduce the risk of feline sarcomas is to only vaccinate your cats against the diseases they are most likely to be exposed to. You should discuss vaccination with your veterinarian when it comes to the rabies and feline leukemia vaccines. Rabies is required by law in many states. Cats who are indoor only cats may not need to be vaccinated against feline leukemia since this is a disease which is contracted and spread only through direct contact. Care must be taken though when bringing a new cat into your home. Make sure it has been tested for leukemia prior to bringing it into your house. Also, make sure that if your cat is given the 3-year rabies vaccine, it is not re-vaccinated prior to the 3-year interval running out. Feline leukemia can also be spread by touching something (cat or bed, etc.) with the virus and then touching your cats.
USDA Approves Drug to Fight Feline Fibrosarcomas [Mar 2001]
Acemannan Immunostimulant is manufactured by Carrington Laboratories and marketed by Veterinary Products of Phoenix, Arizona. Fibrosarcomas send out fingerlike projections that attach to surrounding tissues. This makes excision by surgery very difficult requiring large amounts of tissue to be cut out. Usually, all of the cancerous cells cannot be excised and the fibrosarcomas reappear after surgery.
The drug, refined from the aloe plant, helps by stimulating the immune system to encapsulate or wrap the tumor up. When the edges are more clearly defined, the tumor is easier to remove. The company marketing the drug, recommends that the cat receive injections in both the body and the tumor, before and after surgery, and that the treatment should also include radiation therapy. Carravet Acemannan Immunostimulant lacks the side effects of chemotherapy and so far no adverse effects have been reported.
Since the drug has just been fully licensed, there is no true history as to whether it works or doesn’t work.
Update [April 2004]
Feline fibrosarcomas are also associated with any injection that is given repeatedly such as penicillin or steroid injections. Fibrosarcomas are generally associated with the vaccines and other medications that contain adjuvants (an additive that enhances the effectiveness of a medical treatment).
1 – Task Force of American Animal Hospital Association (AAHA) and the American Association of Feline Practitioners (AAFP). Article from the Journal of Feline Medicine and Surgery (2020) 22, 813-830.
2 – Merck Veterinary Manual, fifth ed., Merck and Co., Inc., Rahway, NJ, 1979, pp. 280-284, 324-327, 330-331, 631-633.
Information on this site is for general information purposes only and is provided without warranty or guarantee of any kind. This site is not intended to replace professional advice from your own veterinarian and nothing on this site is intended as a medical diagnosis or treatment. Any questions about your animal’s health or diet should be directed to your veterinarian.
© 2022 Feline Nutrition Center. All Rights Reserved.
Privacy | Terms